Psoriasis IN Burbank, CA
What is it?
Psoriasis is a chronic, genetic and non-contagious disorder that can affect any area of the body in various forms. The most commonly affected areas include the scalp, elbows, knees, hands, feet, and genitals. Psoriasis causes cells to build up rapidly on the surface of the skin, forming thick silvery scales and itchy, dry, red patches that are sometimes painful. Psoriasis is a persistent, long-lasting (chronic) disease. You may have periods when your psoriasis symptoms improve or go into remission alternating with times your psoriasis worsens.
Several types of psoriasis exist. These include:
Plaque Psoriasis
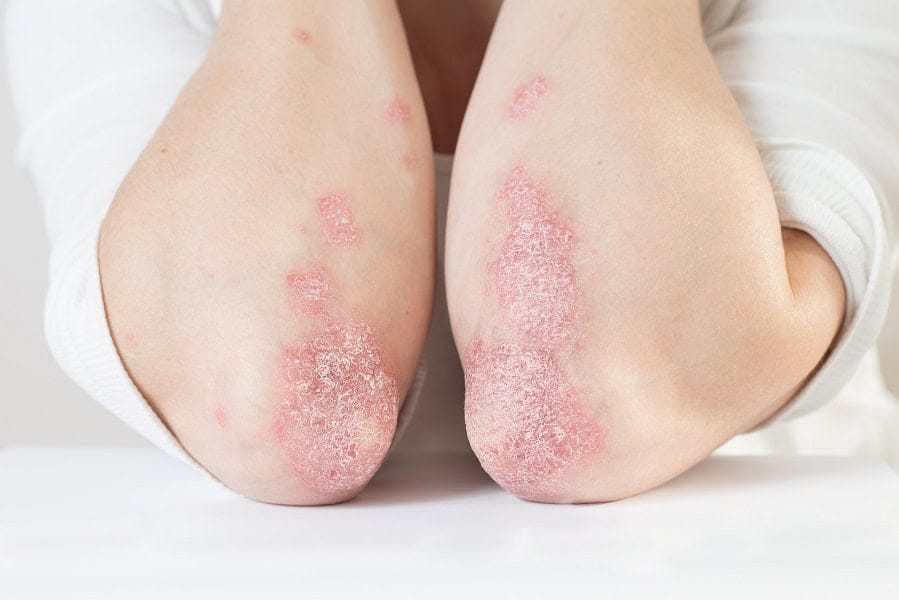
The most common form, plaque psoriasis causes dry, raised, red skin lesions covered with silvery scales. The plaques itch or may be painful and can occur anywhere on your body, including your genitals and the soft tissue inside your mouth. You may have just a few plaques or many, and in severe cases, the skin around your joints may crack and bleed.
Guttate Psoriasis
This primarily affects people younger than 30 and is usually triggered by a bacterial infection such as strep throat. It’s marked by small, water-drop-shaped sores on your trunk, arms, legs and scalp. The sores are covered by a fine scale and aren’t as thick as typical plaques are. You may have a single outbreak that goes away on its own, or you may have repeated episodes, especially if you have ongoing respiratory infections.
Inverse Psoriasis
Mainly affecting the skin in the armpits, groin, under the breasts and around the genitals, inverse psoriasis causes smooth patches of red, inflamed skin. It’s more common in overweight people and is worsened by friction and sweating.
Pustular Psoriasis
This uncommon form of psoriasis can occur in widespread patches or in smaller areas on your hands, feet or fingertips. It generally develops quickly, with pus-filled blisters appearing just hours after your skin becomes red and tender. The blisters dry within a day or two but may reappear every few days or weeks. Generalized pustular psoriasis can also cause fever, chills, severe itching and fatigue.
FAQ'S
Although a cause has not directly been linked to psoriasis, research indicates that some disease triggers can include emotional stress, skin injury, infections, and certain medications. Some people are born with a genetic tendency and are predisposed to the condition, although not everyone with psoriasis has a family history of the condition. Further research attributes the condition to the abnormality of white blood cells in the blood stream that triggers inflammation. This inflammation may also be associated with arthritic, cardiovascular disease if the patient has diabetes mellitus type II.
The best way to prevent the onset of psoriasis is to moisturize regularly, avoid excessive sunlight, take care of your body to avoid infections, reduce emotional and physical stress and monitor any prescription drugs for possible side effects.
